Sore Throat
Everything Science-Based Parents Should Know About Throat Pain - when to worry, when to wait, and how to best manage without over-treating
Reminder: This post is for educational purposes only and does not constitute medical advice. Always consult your child’s pediatric team for guidance specific to your child’s situation.
Sore throats are one of the most common reasons parents call the pediatrician’s office. They’re also one of the most misunderstood.
Most of the time, a sore throat is exactly what it looks like: a virus doing its thing, your kid’s immune system doing its job, and time doing the rest.
No antibiotic needed.
No urgent visit required.
But sometimes a sore throat is something more. Knowing the difference — not just whether it’s strep, but the full picture of what can cause throat pain, how it behaves, what to look for, and when to act — is the kind of knowledge that turns a panicked parent into a confident one.
I wrote this guide so you, dear parent, know the ins and outs of sore throats.
It’s 8 chapters long and covers just about everything I know about sore throats, and I hope it helps you have more confidence all year long.
What’s Covered:
Chapter 1: Why does your throat actually hurt? Main pathways (inflammation, swelling, etc.) that lead to pain so you understand what causes pain.
Chapter 2: Most Sore Throats Are Viral The viruses behind the majority of throat pain, how they behave, and the one clinical clue that usually separates viral from bacterial (and a bunch of different viruses and how they present)
Chapter 3: White Patches Don’t Mean Strep The exudate myth, why visual diagnosis often fails, and why testing make sense
Chapter 4: Strep Throat — What It Is, What It Isn’t, and Why We Actually Treat It The real reason we care about strep, the treatment window, testing options, and the truth about recurring strep and tonsillectomy.
Chapter 5: Mono — The Sore Throat That Doesn’t Quit EBV, the amoxicillin rash trap, spleen rupture, and why fatigue can last months.
Chapter 6: Scarlet Fever and What to Watch For Why Scarlet Fever isn’t as scary as it sounds, how to distinguish it from Kawasaki disease, and what the rash is actually telling you.
Chapter 7: The Life-Threatening Causes of Sore Throat That Aren’t Strep Peritonsillar abscess, retropharyngeal abscess, epiglottitis, bacterial tracheitis, and the red flags that mean go now.
Chapter 8: The Parent’s Decision Framework — When to Call, When to Wait, When to Go A practical guide to using everything in this post when your kid wakes up at 2am with a sore throat.
Chapter 1: Why Does a Sore Throat Actually Hurt?
Before we talk about what’s causing your child’s sore throat, it helps to understand what’s happening in the tissue. The pain your kid is feeling is real and specific. There are actually several distinct mechanisms behind it — and understanding them changes how you think about treatment, timing, and what to expect.
The Throat Is A Complicated Space
Most parents think of the throat as a simple passage: air goes down, food goes down, germs come up. But the pharynx — the back of the throat — is one of the most immunologically active real estate in the human body. It’s lined with mucous membranes, packed with immune tissue, wired with sensory nerves, and sitting right at the crossroads of everything your child breathes, eats, and drinks.
That’s why it gets hit so often. And that’s why, when something goes wrong there, it hurts.
There isn’t one single cause of throat pain. There are several, often occurring simultaneously. Let’s walk through each one.
Mechanism 1: Direct Mucosal Inflammation
The most fundamental cause of throat pain is inflammation of the mucous membrane lining the pharynx.
When a virus or bacterium lands on that tissue, immune cells flood the area. They release a cascade of signaling molecules that do several things at once: they dilate local blood vessels (causing redness and warmth), they increase vascular permeability (causing swelling), and they directly activate the pain-sensing nerve fibers woven throughout the mucosal tissue.
The pain fibers in the pharynx don’t distinguish between viral and bacterial causes. They fire in response to the inflammatory environment. This is why strep and adenovirus can feel identical. The pathogen is different (keep reading below). The downstream inflammation that triggers pain is the same type of process.
This is also why ibuprofen works so well for throat pain: it blocks prostaglandin production, cutting off one of the main pain-signaling pathways. It doesn’t treat the infection. It quiets the inflammation that’s making the nerve endings scream.
Here’s what it looks like when I see these kids: a 6-year-old comes in and can barely swallow her own saliva. The throat looks angry and red — not because there’s any pus or bacterial invasion happening in the tissue, just intense mucosal swelling. Rapid strep test is negative. This is pure viral mucosal inflammation. We give a dose of ibuprofen in the office and fifteen minutes later she’s asking if she can have a Popsicle. That’s prostaglandin blockade doing its job.
Mechanism 2: Tonsillar Swelling
The tonsils are lymphoid organs. Their job is to sample everything coming through the throat — viruses, bacteria, food particles, allergens — and mount an immune response when something looks threatening.
When they’re actively fighting an infection, they swell. Sometimes dramatically. Tonsils that are enlarged enough can make swallowing feel like pushing food through too small a space. In severe cases, they can even begin to encroach on the airway.
Tonsillar swelling contributes to throat pain in two ways. First, the tissue itself is inflamed and tender — the same prostaglandin-driven process as mucosal inflammation, just happening in a larger, denser tissue. Second, the physical bulk of swollen tonsils creates pressure and distortion in the posterior oropharynx, which the brain interprets as pain and discomfort even independent of the inflammatory signaling.
This is why some kids with throat infections feel like something is “stuck” in their throat, or have an unusual quality to their voice, or refuse to eat anything solid. The tonsils are just very large and very unhappy.
Mechanism 3: Lymph Node Enlargement and Referred Pain
The anterior cervical lymph nodes — the chain that runs along the front of the neck, roughly under the jaw and down toward the collarbone — drain the tonsils and posterior pharynx. When the throat is infected, these nodes are doing active immune work: filtering pathogens, coordinating lymphocyte responses, and generating local inflammation of their own.
Enlarged lymph nodes are tender because the capsule surrounding them is being stretched by the swelling inside. That tenderness is perceived as neck pain, jaw pain, or ear pain — not just throat pain. Many parents bring in a child complaining of ear pain and are surprised when the exam shows the ears are perfectly normal; the pain is being referred from inflamed cervical lymph nodes through shared nerve pathways.
This referred pain pattern is important to understand because it can make parents (and even clinicians) suspect ear infection when the primary problem is entirely in the throat.
Here’s what I see: a parent brings in a 5-year-old saying “she keeps grabbing her ear.” I look at the ears — clean and normal. I look at the throat — red, swollen tonsils, tender nodes under the jaw. The ear pain is referred. The throat is the source. Once we treat the pharyngitis, the ear pain resolves.
Mechanism 4: Postnasal Drip and Mucosal Irritation
This is the mechanism most parents overlook entirely. A significant portion of pediatric “sore throats” — especially the mild, chronic, recurrent ones — are not pharyngeal infections at all. They’re the result of nasal secretions draining down the back of the throat.
Here’s how it works. The nose produces mucus constantly. Normally, most of it drains forward and is cleared by the mucociliary system. During a cold or allergic rhinitis flare, mucus production increases significantly and the consistency changes. More of it drains backward: down the posterior nasal passages, across the nasopharynx, and onto the posterior pharyngeal wall.
That drainage is mildly acidic and contains inflammatory mediators from the upper airway. When it sits on the posterior pharyngeal mucosa overnight — especially in a child breathing through the mouth because of nasal congestion — it creates low-grade mucosal irritation. The child wakes up with a scratchy, sore throat. It often feels worst in the morning and improves through the day as the child swallows, drinks fluids, and the drainage pattern changes with upright posture.
This is an extremely common presentation. It’s also one that rarely needs any intervention beyond treating the nasal congestion: saline rinses, a humidifier, adequate hydration, and sometimes an antihistamine if allergy is driving the drainage.
Here’s the clinical scenario I see constantly: a parent calls because their child has had a sore throat “every morning for the past three weeks.” I ask a few questions — does it get better after breakfast? Is there a runny nose or congestion? Does the child snore? Is it allergy season? Often all four are yes. This is postnasal drip doing exactly what postnasal drip does. A rapid strep test would almost certainly be negative. The throat doesn’t need antibiotics. The nose needs attention.
Mechanism 5: Dry Air and Mouth Breathing
Related to postnasal drip but worth its own section: dry air and mouth breathing cause a distinct type of throat discomfort that has nothing to do with infection.
The throat mucosa is designed to stay moist. Mucous glands in the lining constantly secrete a thin protective layer that keeps the tissue hydrated and helps trap inhaled particles. When a child breathes through the mouth — because of nasal congestion, tonsillar hypertrophy, habit, or sleeping on their back — that moisture evaporates. The mucosal surface becomes dry, slightly cracked, and hypersensitive.
Dry winter air makes this worse. Forced-air heating systems drop indoor humidity dramatically. A child sleeping in a room with 20% relative humidity is essentially running an evaporative drying process on their pharyngeal mucosa for 10 hours straight.
The resulting throat discomfort is real. It’s not infection-related. It doesn’t respond to antibiotics. It responds to: a cool-mist humidifier in the room at night, ensuring the child is well-hydrated before bed, treating the nasal congestion that’s forcing mouth breathing in the first place, and sometimes a small sip of warm water or honey in the morning to coat the mucosa.
Putting It Together: Why the Same Symptom Has So Many Different Causes
When your child says “my throat hurts,” that’s a single symptom pointing to at least seven distinct physiological mechanisms — sometimes several operating simultaneously. A child with a cold and significant nasal congestion might have mucosal inflammation from the virus, postnasal drip irritating the posterior wall, and mouth-breathing dryness all at once. A child with strep has direct bacterial tissue invasion driving intense mucosal inflammation plus tonsillar swelling plus lymph node activation producing referred ear and jaw pain.
Understanding this matters for two reasons.
First, it explains why throat pain intensity doesn’t reliably predict the cause. A child with a purely viral sore throat and no bacterial component can have excruciating pain. A child with confirmed strep can have surprisingly mild discomfort. The severity of the pain reflects the total inflammatory load — from all these mechanisms combined — not the specific pathogen.
Second, it clarifies why treatment has to match the mechanism. Antibiotics only address one of these pathways: direct bacterial infection. For every other mechanism on this list, antibiotics do nothing. The tools that work for postnasal drip, dry air, reflux, and nerve sensitization are entirely different. And yet “sore throat” as a complaint often reflexively leads to antibiotic conversations, even when the underlying mechanism has nothing to do with bacteria.
That context — what’s actually happening in the tissue — is the foundation for everything in the chapters that follow.
Chapter 2: Most Sore Throats Are Viral
Here’s the stat that most parents find surprising: group A strep, the bacteria behind strep throat, accounts for only about 15% of all sore-throat cases in kids. That means 85% of the time, the cause is something else. The vast majority of the time, that something else is a virus.
This is actually good news. Viruses don’t respond to antibiotics. Which means most kids with a sore throat don’t need one. No antibiotic, no side effects, no contribution to antibiotic resistance. The immune system handles it, the throat recovers, and everyone moves on.
The harder part is sitting with the uncertainty. When your child is miserable and you’re staring at a red, swollen throat at 11pm, “it’s probably a virus” doesn’t feel reassuring…instead it leaves a lot of “what ifs” and “what will tomorrow look like”. Understanding what’s actually going on changes that. It gives you a framework instead of uncertainty.
Which viruses cause sore throats?
A lot of them. Parainfluenza and influenza viruses, rhinoviruses (classic cold viruses), coronaviruses, respiratory syncytial virus (RSV), adenovirus, enteroviruses like coxsackievirus and echovirus, herpes simplex virus, and Epstein-Barr virus. All of these can cause pharyngitis, which is just the medical term for throat inflammation. Each one has its own personality.
With parainfluenza, influenza, rhinoviruses, coronaviruses, and RSV, the sore throat is usually mild and gets overshadowed by the rest of the upper respiratory picture: runny nose, congestion, cough. The throat hurts, but it’s not the main event. Typically we see the throat pain after a day or two of runny nose and congestion. The mucus drainage from the nose, dry air from mouth breathing, (scroll back up to chapter 1 for a refresher)
Influenza is its own beast. High fever, cough, headache, body aches, real malaise. Kids with flu look like they got hit by a truck. Pharyngitis is part of the picture, but so is everything else.
Adenovirus is a convincing impersonator of bacterial illness. It produces fever, real redness in the throat, follicular changes on the tonsils, exudate (yes, white patches — more on this in Chapter 2), and swollen lymph nodes. When conjunctivitis shows up alongside the pharyngitis, we call it pharyngoconjunctival fever, a distinct adenoviral syndrome. Lab work can show elevated white counts and elevated inflammatory markers, exactly what you’d expect from a bacterial infection. And yet it’s a virus. Antibiotics won’t touch it. It runs its course over about a week.
Here’s what it looks like when I see these kids: an 8-year-old comes in with two days of fever, a red throat with some white patches, and swollen neck glands. The rapid strep test is negative. But look closer — there’s some puffiness around the eyes, a little redness in the conjunctiva. Maybe a mild cough. That’s adenovirus until proven otherwise. The parents are convinced it’s strep because of the exudate. I have to walk them through why we trust the test, not the visual.
This matters because adenovirus is one of the biggest drivers of antibiotic overprescription. It looks bacterial. It doesn’t act bacterial. And it doesn’t respond to antibiotics.
Enteroviruses: summer throat pain.
Coxsackievirus and echovirus tend to show up in summer. High fever, red throat, but usually without the exudate and lymph node swelling you’d see with strep. Symptoms resolve within a few days.
Two specific enterovirus syndromes are worth knowing:
Herpangina causes distinctive painful, gray-white lesions in the back of the throat. The vesicles start small, surrounded by red halos, then ulcerate. Fever can spike high. Pain can be severe enough to interfere with drinking.
Hand-foot-mouth disease, caused by coxsackievirus A16, causes vesicles throughout the mouth and on the palms, soles, and sometimes the trunk. Fever is common. Most kids don’t look seriously ill. Both conditions typically resolve in less than a week, but hydration can be a real challenge in the meantime.
Here’s what it looks like when I see these kids: a 3-year-old in July who’s been refusing food and drink for two days, drooling a little, running a fever around 103. Mom lifts his upper lip and you can see tiny ulcers on the inside of his cheeks. He’s got a few vesicles on his palms. Classic hand-foot-mouth. The conversation is entirely about hydration, pain management, and what to watch for. There’s nothing a prescription will fix here.
The clue that usually points to viral.
The most clinically useful thing to know: when sore throat comes with conjunctivitis, rhinitis, cough, discrete ulcers, hoarseness, croup, or diarrhea, the cause is almost certainly viral. If the sore throat came after a day or few of runny nose, it’s usually from inflammation and drainage rather than strep. These features are common in viral pharyngitis and rare in bacterial pharyngitis.
Chapter 3: White Patches Don’t Always Mean Strep
Let’s clear this up immediately, because it drives a lot of unnecessary treatment.
White patches on the tonsils, the technical term is tonsillar exudate, do not mean strep throat. They are not diagnostic of bacterial infection. They do not require antibiotics.
Exudate is simply a sign of significant tonsil inflammation. And significant tonsil inflammation can happen with viruses too. Adenovirus does it. Epstein-Barr virus (mono) does it. Even some enteroviral infections can produce exudate.
Here’s what I see in clinic: a parent comes in convinced their child has strep because “the back of the throat is full of white stuff.” And I understand the logic. White patches look infected. They look like something needs to be killed. But I’ve seen plenty of confirmed viral pharyngitis with dramatic exudate, and plenty of confirmed strep with a relatively unremarkable-looking throat. The visual just isn’t reliable.
In fact, among kids who get tested, plenty with dramatic white patches test negative for strep. And plenty who test positive have throats that look almost normal.
The visual appearance of the throat is notoriously unreliable for distinguishing viral from bacterial pharyngitis. This has been studied extensively, and the conclusion is consistent: no combination of clinical features is accurate enough to diagnose or rule out strep without a test.
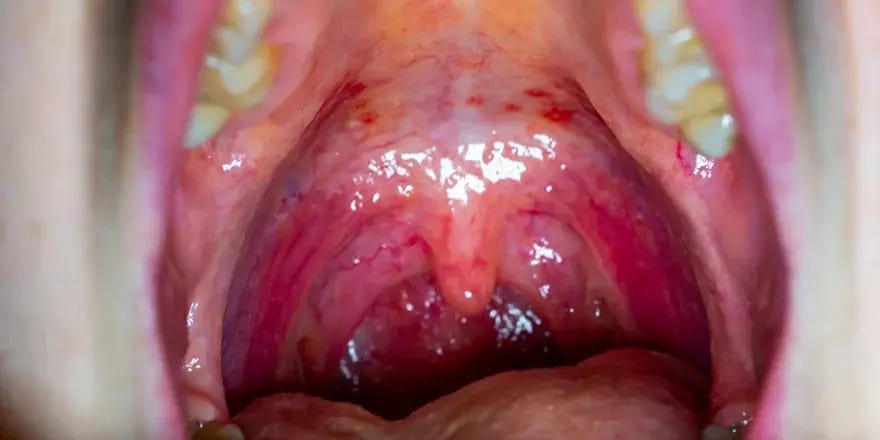
So what does strep actually look like?
Classic strep pharyngitis presents with sudden onset of fever and sore throat. Headache, stomach pain, nausea, and vomiting are common and sometimes leading symptoms that bring kids in. The tonsils are enlarged, red, and symmetric, sometimes with patchy exudates. The palate may have small red spots called petechiae. The anterior cervical lymph nodes, the ones right under the jaw toward the front of the neck, are often tender and enlarged. Infrequently, the tongue may look red and bumpy: the classic “strawberry tongue.”
What you generally won’t see with strep: runny nose, cough, conjunctivitis, hoarseness, diarrhea, or mouth ulcers. When those are present, the picture is almost certainly viral.
But here is the critical point: even the most classic-looking strep presentation needs a test. Physicians who rely on clinical impression alone consistently overestimate the probability of strep. The only reliable way to know is a rapid strep test, a throat culture, or a molecular PCR-based test.
The scoring system doctors use and its limitations.
Pediatricians often use something called either the Centor Score or McIsaac score to estimate the probability of strep before testing. The criteria: fever above 101°C, tender anterior cervical lymph nodes, tonsillar swelling or exudate, absence of cough, and age 3-15 years. One point for each.
At the highest scores, the chance of having strep is about 45-62%. That’s better than chance, but it’s still far from certain. At lower scores, the negative predictive value is around 80%: a low score makes strep fairly unlikely, but not impossible.
The takeaway: scoring systems help, but they don’t replace testing.
What happens when you skip the test and just treat?
A few things.
First, about 85% of the time you’re treating a virus with an antibiotic that can’t touch it, exposing your kid to side effects (diarrhea, rash, allergic reactions, gut microbiome disruption) for no benefit.
Keep reading with a 7-day free trial
Subscribe to dear parents to keep reading this post and get 7 days of free access to the full post archives.

